Keratoacanthoma.
KA is a rapidly growing scaly nodule that mimics Squamous Cell Carcinoma.
KA is a rapidly growing scaly nodule that mimics Squamous Cell Carcinoma.
Keratoacanthoma (or simply ‘KA’) is a benign tumour of the sebaceous gland that develops as a red or skin-coloured spot and grows rapidly over a few weeks. Rarely, keratoacanthoma itself may develop into an invasive SCC. Experts believe that a KC is in fact a type of well-differentiated (or “mild”) squamous cell carcinoma.
Keratoacanthoma typically affects older people who have fair, sun-exposed skin. However, KA can appear at any age, especially if immunosuppressants have been used.
Keratoacanthoma has many similarities with SCC (Squamous Cell Carcinoma) and is often very difficult to tell apart, both clinically and pathologically.
KA generally occurs on sun-exposed sights such as the outside of the ears, parts of the face, the back of hands and forearms, and the lower limb.
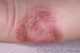
The lesion is usually pink, light brown or skin coloured. It grows away from the skin in the shape of a dome. KA usually grows to between 1 and 3cm in size, by which time it has a central crusted plug, giving it the classical description of a volcano. Even without a crust, you will feel the scale on a KA.
It’s almost impossible to be clinically certain that a KA is not an SCC – the appearances are very similar even with a dermatoscope.
Gallery of Keratoacanthoma
Keratoacanthomas typically turn into scar tissue over time. It is generally not considered safe to “wait and see.” The rationale for removing a Keratoacanthoma is:
Keratoacanthomas are usually excised through formal excision, which ensures the lesion is removed completely. A margin of at least 3mm is ideal. By removing the entire depth of the lesion, the pathologist has the best chance of excluding SCC.
Other treatment options may be considered (depending on the circumstance & discussion with the patient) such as curettage and cautery. The curettage must, however, be performed deeply so as to ensure the entire depth of the lesion is treated. It may take several weeks for the wound to heal, another reason formal excision is usually preferred. Medical treatments include the injection of a chemotherapeutic agent.
There are some of the key terms that may be found in the pathology report.
A keratoacanthoma & Squamous Cell carcinoma may look similar – at first glance – to the pathologist. It is helpful for the pathology specimen to include the base of the lesion.
Central Core
Keratoacanthoma typically has a central core like a Volcano. You can see this in the photos. This core consists mainly of keratin.
Well differentiated Keratinocytes
The keratinocytes (the main skin cells normally found in the lowest layer of the epidermis) look fairly normal. They may contain “glassy eoesinophilic cytoplasm” – these are pale glassy coloured cells.
Mixed inflammatory infiltrate
There may be inflammatory cells underneath the KA. The different types of inflammatory cells found are lymphocytes, neutrophils &/or Eosinophils.
In practical terms, KA is best diagnosed by a pathologist.
 ©South East Skin Clinic, All rights reserved
©South East Skin Clinic, All rights reserved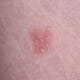 ©South East Skin Clinic, All rights reservedIEC (Intraepidermal Carcinoma)
©South East Skin Clinic, All rights reservedIEC (Intraepidermal Carcinoma)